When our patient was admitted, we administered an infusion of 2400 U (40 U/kg) of factor VIII. Since the 1960s, the mortality of ICH has declined from 70 to 20%. Prophylaxis is effective in decreasing the incidence risk of ICH.
īecause of its etiology, hemophilia A requires treatment with factor VIII. Frequently, the pathogenesis of ICH is unknown. ICH can occur spontaneously or after trauma it may also be caused by other risk factors (e.g., severe diseases and infection). ICH, one of the most serious and life-threatening events, is relatively rare in patients with hemophilia. ICH and joint destruction are the two most important late complications observed patients with hemophilia. Mild hemophilia is observed with bleeding in response to injury or surgery, such as bleeding of the teeth or mucous bleeding, mainly later in life. The diagnoses of SDH and hemophilia A were confirmed. A CT scan was performed upon his arrival to the hospital to evaluate his illness. Once the patient was admitted, normal treatment to reduce intracranial pressure was administered.
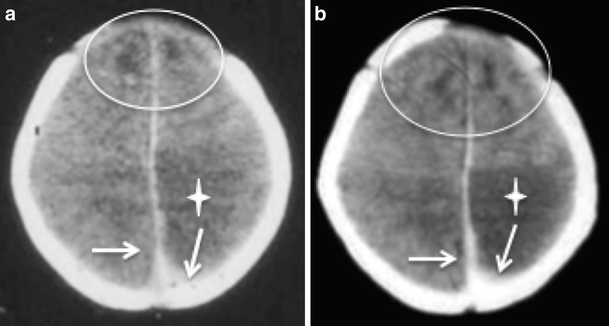
Patients with severe hemophilia rarely exhibit mild clinical signs but can present with normal von Willebrand factor antigen levels, platelet counts, and prothrombin times. However, APTT might be normal in mild factor deficiencies. Normally, a prolonged APTT increases as hemophilia severity worsens. Because of his clinical history of hemophilia A and the severity of the disease, we measured his factor VIII activity levels in an APTT-based assay (APTT prolongation time). He was admitted to the emergency room following a diagnosis of SDH. Our patient was a middle-aged male who had inherited hemophilia A. Monitoring coagulation function is also important during the perioperative period. Primary treatment for hemophilia A is infusion of sufficient factor VIII and an emergency operation. A prolonged APTT is a factor used to identify hemophilia. Hemophilia A, which occurs in approximately 1 in 5000 live male births, is more common and more likely to be severe, and morbidity is higher among males than among females. Hemophilia is classified as severe (factor level < 0.01 IU/ml), moderate (factor level < 0.05 IU/ml), and mild (factor level ≥ 0.05 and < 0.4). Hemophilia is an inherited bleeding disorder that can be classified into three types based on deficiency of the following coagulation factors: factor VIII (hemophilia A), factor IX (hemophilia B), and factor XI (hemophilia C). Cranioplasty was required after 6–12 months. He had a follow-up visit 3 months after discharge, and right oculomotor and right eye movements were observed. Myodynamia had recovered, and the Babinski sign was negative on both sides. The right oculomotor nerve showed paralysis with ptosis, and the diameter of the pupil was 5 mm. The APTT was 55.5 s, and the international normalized ratio was 1.16. When he was released from the hospital, factor VIII inhibitor was 0, and factor VIII activity was 25.9%. The APTT was 34–57 s 2 weeks after the operation. We continued to infuse 2400 U of factor VIII per 12 h for the first 3 days after surgery, 1600 U per 12 h from the 4th day to the 1st week, and 1000 U per day from the 1st week to the 2nd week. Based on the consultations, we infused the patient with 2400 U (40 U/kg) of factor VIII during the operation. Preoperative and postoperative CT scans are shown in Fig. The operation proceeded normally, and the amount of bleeding was 4 U. We agreed that infusing sufficient factor VIII was the most important factor in the perioperative period. We held consultations in the Hematology Department, intensive care unit, and Anesthesiology Department. The patient received a 250-ml infusion of mannitol as soon as he was admitted. The hematoma volume was approximately 60 ml. A computed tomography (CT) scan showed right acute parietal and frontotemporal SDH with a 15-mm midline shift. The activated partial thromboplastin time (APTT) was increased to 103.4 s, factor VIII inhibitor was 0, and fibrinogen was decreased to 1.64 g/L. The patient had hypermyotonia with an absence of myodynamia, and the Babinski sign was positive on both sides. The light reflex was absent in the right eye and diminished in the left.

The diameters of the left and right pupil were 4 mm and 6 mm, respectively. On arrival, the patient’s Glasgow Coma Score was 6/15. Due to a lack of factor VIII in the admitting hospital, he was transferred to our hospital. The patient’s medical history was normal, except for hemophilia A. A 56-year-old man went into a coma after presenting with a headache and vomiting spontaneously 8 h before he was admitted to the hospital.
